General Information About Plasma Cell Neoplasms
Plasma cell neoplasms are diseases in which the body makes too many plasma cells.
Plasma cells develop from B lymphocytes (B cells), a type of white blood cell that is made in the bone marrow. Normally, when bacteria or viruses enter the body, some of the B cells will change into plasma cells. The plasma cells make antibodies to fight bacteria and viruses, to stop infection and disease.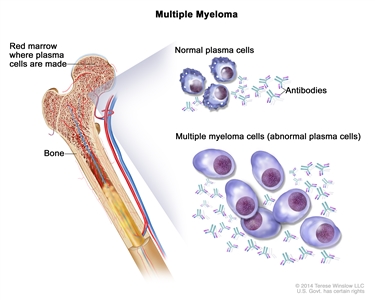
Multiple myeloma. Multiple myeloma cells are abnormal plasma cells (a type of white blood cell) that build up in the bone marrow and form tumors in many bones of the body. Normal plasma cells make antibodies to help the body fight infection and disease. As the number of multiple myeloma cells increases, more antibodies are made. This can cause the blood to thicken and keep the bone marrow from making enough healthy blood cells. Multiple myeloma cells also damage and weaken the bone.
Plasma cell neoplasms are diseases in which abnormal plasma cells form tumors in the bones or soft tissues of the body. The plasma cells also make an antibody protein, called M protein, that is not needed by the body and does not help fight infection. These antibody proteins build up in the bone marrow and can cause the blood to thicken or can damage the kidneys.
Plasma cell neoplasms can be benign (not cancer) or malignant (cancer).
Monoclonal gammopathy of undetermined significance (MGUS) is not cancer but can become cancer. The following types of plasma cell neoplasms are cancer:
- Lymphoplasmacytic lymphoma (also called Waldenström macroglobulinemia). For more information, see Non-Hodgkin Lymphoma Treatment.
- Plasmacytoma.
- Multiple myeloma.
There are several types of plasma cell neoplasms.
Plasma cell neoplasms include the following:
Monoclonal gammopathy of undetermined significance (MGUS)
In this type of plasma cell neoplasm, less than 10% of the bone marrow is made up of abnormal plasma cells and there is no cancer. The abnormal plasma cells make M protein, which is sometimes found during a routine blood or urine test. In most patients, the amount of M protein stays the same and there are no signs, symptoms, or health problems.
In some patients, MGUS may later become a more serious condition, such as amyloidosis, or cause problems with the kidneys, heart, or nerves. MGUS can also become cancer, such as multiple myeloma, lymphoplasmacytic lymphoma, or chronic lymphocytic leukemia.
Plasmacytoma
In this type of plasma cell neoplasm, the abnormal plasma cells (myeloma cells) are in one place and form one tumor, called a plasmacytoma. Sometimes plasmacytoma can be cured. There are two types of plasmacytoma.
- In isolated plasmacytoma of bone, one plasma cell tumor is found in the bone, less than 10% of the bone marrow is made up of plasma cells, and there are no other signs of cancer. Plasmacytoma of the bone often becomes multiple myeloma.
- In extramedullary plasmacytoma, one plasma cell tumor is found in soft tissue but not in the bone or the bone marrow. Extramedullary plasmacytomas commonly form in tissues of the throat, tonsil, and paranasal sinuses.
Signs and symptoms depend on where the tumor is.
- In bone, the plasmacytoma may cause pain or broken bones.
- In soft tissue, the tumor may press on nearby areas and cause pain or other problems. For example, a plasmacytoma in the throat can make it hard to swallow.
Multiple myeloma
In multiple myeloma, abnormal plasma cells (myeloma cells) build up in the bone marrow and form tumors in many bones of the body. These tumors may keep the bone marrow from making enough healthy blood cells. Normally, the bone marrow makes stem cells (immature cells) that become three types of mature blood cells:
- Red blood cells that carry oxygen and other substances to all tissues of the body.
- White blood cells that fight infection and disease.
- Platelets that form blood clots to help prevent bleeding.
As the number of myeloma cells increases, fewer red blood cells, white blood cells, and platelets are made. The myeloma cells also damage and weaken the bone.
Sometimes multiple myeloma does not cause any signs or symptoms. This is called smoldering multiple myeloma. It may be found when a blood or urine test is done for another condition. Signs and symptoms may be caused by multiple myeloma or other conditions. Check with your doctor if you have any of the following:
- Bone pain, especially in the back or ribs.
- Bones that break easily.
- Fever for no known reason or frequent infections.
- Easy bruising or bleeding.
- Trouble breathing.
- Weakness of the arms or legs.
- Feeling very tired.
A tumor can damage the bone and cause hypercalcemia (too much calcium in the blood). This can affect many organs in the body, including the kidneys, nerves, heart, muscles, and digestive tract, and cause serious health problems.
Hypercalcemia may cause the following signs and symptoms:
- Loss of appetite.
- Nausea or vomiting.
- Feeling thirsty.
- Frequent urination.
- Constipation.
- Feeling very tired.
- Muscle weakness.
- Restlessness.
- Confusion or trouble thinking.
Multiple myeloma and other plasma cell neoplasms may cause a condition called amyloidosis.
In rare cases, multiple myeloma can cause peripheral nerves (nerves that are not in the brain or spinal cord) and organs to fail. This may be caused by a condition called amyloidosis. Antibody proteins build up and stick together in peripheral nerves and organs, such as the kidney and heart. This can cause the nerves and organs to become stiff and unable to work the way they should.
Amyloidosis may cause the following signs and symptoms:
- Feeling very tired.
- Purple spots on the skin.
- Enlarged tongue.
- Diarrhea.
- Swelling caused by fluid in your body's tissues.
- Tingling or numbness in your legs and feet.
Age can affect the risk of plasma cell neoplasms.
Anything that increases a person's chance of getting a disease is called a risk factor. Not every person with one or more of these risk factors will develop plasma cell neoplasms, and they will develop in people who don't have any known risk factors. Talk with your doctor if you think you may be at risk.
Plasma cell neoplasms are most common in people who are middle aged or older. For multiple myeloma and plasmacytoma, other risk factors include the following:
- Being Black.
- Being male.
- Having a personal history of MGUS or plasmacytoma.
- Being exposed to radiation or certain chemicals.
Studies about how racial, social, and financial factors affect access to treatment and rates of plasma cell neoplasms are ongoing.
Tests that examine the blood, bone marrow, and urine are used to diagnose multiple myeloma and other plasma cell neoplasms.
In addition to asking about your personal and family health history and doing a physical exam, your doctor may perform the following tests and procedures:
-
Blood and urine immunoglobulin studies: A procedure in which a blood or urine sample is checked to measure the amounts of certain antibodies (immunoglobulins). For multiple myeloma, beta-2-microglobulin, M protein, free light chains, and other proteins made by the myeloma cells are measured. A higher-than-normal amount of these substances can be a sign of disease.
-
Bone marrow aspiration and biopsy: The removal of bone marrow, blood, and a small piece of bone by inserting a hollow needle into the hipbone or breastbone. A pathologist views the bone marrow, blood, and bone under a microscope to look for abnormal cells.
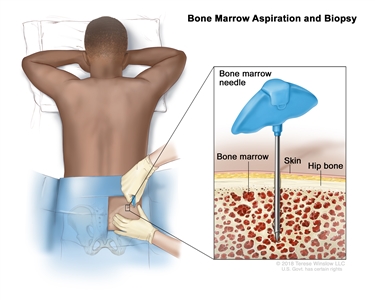
Bone marrow aspiration and biopsy. After a small area of skin is numbed, a long, hollow needle is inserted through the patient's skin and hip bone into the bone marrow. A sample of bone marrow and a small piece of bone are removed for examination under a microscope. The following tests may be done on the sample of tissue removed during the bone marrow aspiration and biopsy: - Cytogenetic analysis: A laboratory test in which the chromosomes of cells in a sample of bone marrow are counted and checked for any changes, such as broken, missing, rearranged, or extra chromosomes. Changes in certain chromosomes may be a sign of cancer. Cytogenetic analysis is used to help diagnose cancer, plan treatment, or find out how well treatment is working.
- FISH (fluorescence in situ hybridization): A laboratory test used to look at and count genes or chromosomes in cells and tissues. Pieces of DNA that contain fluorescent dyes are made in the laboratory and added to a sample of a patient's cells or tissues. When these dyed pieces of DNA attach to certain genes or areas of chromosomes in the sample, they light up when viewed under a fluorescent microscope. The FISH test is used to help diagnose cancer and help plan treatment.
- Flow cytometry: A laboratory test that measures the number of cells in a sample, the percentage of live cells in a sample, and certain characteristics of the cells, such as size, shape, and the presence of tumor (or other) markers on the cell surface. The cells from a sample of a patient's bone marrow are stained with a fluorescent dye, placed in a fluid, and then passed one at a time through a beam of light. The test results are based on how the cells that were stained with the fluorescent dye react to the beam of light. This test is used to help diagnose and manage certain types of cancers, such as leukemia and lymphoma.
-
Skeletal bone survey: In a skeletal bone survey, x-rays of all the bones in the body are taken. The x-rays are used to find areas where the bone is damaged. An x-ray is a type of energy beam that can go through the body and onto film, making a picture of areas inside the body.
-
Complete blood count (CBC) with differential: A procedure in which a sample of blood is drawn and checked for the following:
- The number of red blood cells and platelets.
- The number and type of white blood cells.
- The amount of hemoglobin (the protein that carries oxygen) in the red blood cells.
- The portion of the blood sample made up of red blood cells.
-
Blood chemistry studies: A procedure in which a blood sample is checked to measure the amounts of certain substances, such as calcium or albumin, released into the blood by organs and tissues in the body. An unusual (higher or lower than normal) amount of a substance can be a sign of disease.
-
Twenty-four-hour urine test: A test in which urine is collected for 24 hours to measure the amounts of certain substances. An unusual (higher or lower than normal) amount of a substance can be a sign of disease in the organ or tissue that makes it. A higher than normal amount of protein may be a sign of multiple myeloma.
-
MRI (magnetic resonance imaging): A procedure that uses a magnet, radio waves, and a computer to make a series of detailed pictures of areas inside the body. This procedure is also called nuclear magnetic resonance imaging (NMRI). An MRI of the spine and pelvis may be used to find areas where the bone is damaged.
-
PET scan (positron emission tomography scan): A procedure to find malignant tumor cells in the body. A small amount of radioactive glucose (sugar) is injected into a vein. The PET scanner rotates around the body and makes a picture of where glucose is being used in the body. Malignant tumor cells show up brighter in the picture because they are more active and take up more glucose than normal cells do.
-
CT scan (CAT scan): A procedure that makes a series of detailed pictures of areas inside the body, such as the spine, taken from different angles. The pictures are made by a computer linked to an x-ray machine. A dye may be injected into a vein or swallowed to help the organs or tissues show up more clearly. This procedure is also called computed tomography, computerized tomography, or computerized axial tomography.
-
PET-CT scan: A procedure that combines the pictures from a positron emission tomography (PET) scan and a computed tomography (CT) scan. The PET and CT scans are done at the same time with the same machine. The combined scans give more detailed pictures of areas inside the body, such as the spine, than either scan gives by itself.
Certain factors affect prognosis (chance of recovery) and treatment options.
The prognosis depends on the following:
- The type of plasma cell neoplasm.
- The stage of the disease.
- Whether a certain immunoglobulin (antibody) is present.
- Whether there are certain genetic changes.
- Whether the kidney is damaged.
- Whether the cancer responds to initial treatment or recurs (comes back).
Treatment options depend on the following:
- The type of plasma cell neoplasm.
- The age and general health of the patient.
- Whether there are signs, symptoms, or health problems, such as kidney failure or infection, related to the disease.
- Whether the cancer responds to initial treatment or recurs (comes back).
Stages of Plasma Cell Neoplasms
There are no standard staging systems for monoclonal gammopathy of undetermined significance (MGUS) and plasmacytoma.
After multiple myeloma has been diagnosed, tests are done to find out how much cancer is in the body.
The process used to find out the amount of cancer in the body is called staging. It is important to know the stage in order to plan treatment.
The following tests and procedures may be used to find out how much cancer is in the body:
-
Skeletal bone survey: In a skeletal bone survey, x-rays of all the bones in the body are taken. The x-rays are used to find areas where the bone is damaged. An x-ray is a type of energy beam that can go through the body and onto film, making a picture of areas inside the body.
-
MRI (magnetic resonance imaging): A procedure that uses a magnet, radio waves, and a computer to make a series of detailed pictures of areas inside the body, such as the bone marrow. This procedure is also called nuclear magnetic resonance imaging (NMRI).
-
Bone densitometry: A procedure that uses a special type of x-ray to measure bone density.
The stage of multiple myeloma is based on the levels of beta-2-microglobulin and albumin in the blood.
Beta-2-microglobulin and albumin are found in the blood. Beta-2-microglobulin is a protein found on plasma cells. Albumin makes up the biggest part of the blood plasma. It keeps fluid from leaking out of blood vessels. It also brings nutrients to tissues, and carries hormones, vitamins, drugs, and other substances, such as calcium, all through the body. In the blood of patients with multiple myeloma, the amount of beta-2-microglobulin is increased and the amount of albumin is decreased.
The following stages are used for multiple myeloma:
Stage I multiple myeloma
In stage I multiple myeloma, the blood levels are as follows:
- beta-2-microglobulin level is lower than 3.5 mg/L; and
- albumin level is 3.5 g/dL or higher.
Stage II multiple myeloma
In stage II multiple myeloma, the blood levels are in between the levels for stage I and stage III.
Stage III multiple myeloma
In stage III multiple myeloma, the blood level of beta-2-microglobulin is 5.5 mg/L or higher and the patient also has one of the following:
- high levels of lactate dehydrogenase (LDH); or
- certain changes in the chromosomes.
Plasma cell neoplasms may not respond to treatment or may come back after treatment.
Plasma cell neoplasms are called refractory when the number of plasma cells keeps going up even though treatment is given. Plasma cell neoplasms are called relapsed when they have come back after treatment.
Treatment Option Overview
There are different types of treatment for patients with plasma cell neoplasms.
Different types of treatments are available for patients with plasma cell neoplasms. Some treatments are standard (the currently used treatment), and some are being tested in clinical trials. A treatment clinical trial is a research study meant to help improve current treatments or obtain information on new treatments for patients with cancer. When clinical trials show that a new treatment is better than the standard treatment, the new treatment may become the standard treatment. Patients may want to think about taking part in a clinical trial. Some clinical trials are open only to patients who have not started treatment.
The following types of treatment are used:
Chemotherapy
Chemotherapy is a cancer treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. When chemotherapy is taken by mouth or injected into a vein or muscle, the drugs enter the bloodstream and can reach cancer cells throughout the body (systemic chemotherapy).
See Drugs Approved for Multiple Myeloma and Other Plasma Cell Neoplasms.
Other drug therapy
Corticosteroids are steroids that have antitumor effects in multiple myeloma.
Targeted therapy
Targeted therapy is a type of treatment that uses drugs or other substances to identify and attack specific cancer cells. Several types of targeted therapy may be used to treat multiple myeloma and other plasma cell neoplasms. There are different types of targeted therapy:
- Proteasome inhibitor therapy: This treatment blocks the action of proteasomes in cancer cells. A proteasome is a protein that removes other proteins no longer needed by the cell. When the proteins are not removed from the cell, they build up and may cause the cancer cell to die. Bortezomib, carfilzomib, and ixazomib are proteasome inhibitors used in the treatment of multiple myeloma and other plasma cell neoplasms.
- Monoclonal antibody therapy: Monoclonal antibodies are immune system proteins made in the laboratory to treat many diseases, including cancer. As a cancer treatment, these antibodies can attach to a specific target on cancer cells or other cells that may help cancer cells grow. The antibodies are able to then kill the cancer cells, block their growth, or keep them from spreading. Monoclonal antibodies are given by infusion. They may be used alone or to carry drugs, toxins, or radioactive material directly to cancer cells. Daratumumab and elotuzumab are monoclonal antibodies used in the treatment of multiple myeloma and other plasma cell neoplasms. Denosumab is a monoclonal antibody used to slow bone loss and reduce bone pain in patients with multiple myeloma.monoclonal antibodies: how monoclonal antibodies treat cancerHow do monoclonal antibodies work to treat cancer? This video shows how monoclonal antibodies, such as trastuzumab, pembrolizumab, and rituximab, block molecules cancer cells need to grow, flag cancer cells for destruction by the body's immune system, or deliver harmful substances to cancer cells.
- BCL2 inhibitor therapy: This treatment blocks a protein called BCL2. Blocking this protein may help kill cancer cells and may make them more sensitive to anticancer drugs. Venetoclax is a BCL2 inhibitor being studied in the treatment of relapsed or refractory multiple myeloma.
See Drugs Approved for Multiple Myeloma and Other Plasma Cell Neoplasms.
High-dose chemotherapy with stem cell transplant
High doses of chemotherapy are given to kill cancer cells. Healthy cells, including blood -forming cells, are also destroyed by the cancer treatment. Stem cell transplant is a treatment to replace the blood-forming cells. Stem cells (immature blood cells) are removed from the blood or bone marrow of the patient (autologous) or a donor (allogeneic) and are frozen and stored. After the patient completes chemotherapy, the stored stem cells are thawed and given back to the patient through an infusion. These reinfused stem cells grow into (and restore) the body's blood cells. 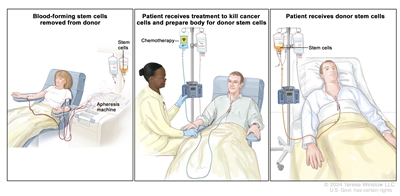
Donor stem cell transplant. (Step 1): Four to five days before donor stem cell collection, the donor receives a medicine to increase the number of stem cells circulating through their bloodstream (not shown). The blood-forming stem cells are then collected from the donor through a large vein in their arm. The blood flows through an apheresis machine that removes the stem cells. The rest of the blood is returned to the donor through a vein in their other arm. (Step 2): The patient receives chemotherapy to kill cancer cells and prepare their body for the donor stem cells. The patient may also receive radiation therapy (not shown). (Step 3): The patient receives an infusion of the donor stem cells.
Immunotherapy
Immunotherapy is a treatment that uses the patient's immune system to fight cancer. Substances made by the body or made in a laboratory are used to boost, direct, or restore the body's natural defenses against cancer. This cancer treatment is a type of biologic therapy.
- Immunomodulator therapy: Thalidomide, lenalidomide, and pomalidomide are immunomodulators used to treat multiple myeloma and other plasma cell neoplasms.
- CAR T-cell therapy: This treatment changes the patient's T cells (a type of immune system cell) so they will attack certain proteins on the surface of cancer cells. T cells are taken from the patient and special receptors are added to their surface in the laboratory. The changed cells are called chimeric antigen receptor (CAR) T cells. The CAR T cells are grown in the laboratory and given to the patient by infusion. The CAR T cells multiply in the patient's blood and attack cancer cells. CAR T-cell therapy is being studied in the treatment of multiple myeloma that has recurred (come back).
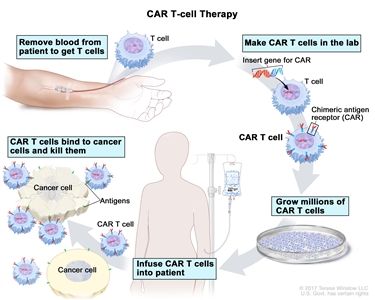
CAR T-cell therapy. A type of treatment in which a patient's T cells (a type of immune cell) are changed in the laboratory so they will bind to cancer cells and kill them. Blood from a vein in the patient's arm flows through a tube to an apheresis machine (not shown), which removes the white blood cells, including the T cells, and sends the rest of the blood back to the patient. Then, the gene for a special receptor called a chimeric antigen receptor (CAR) is inserted into the T cells in the laboratory. Millions of the CAR T cells are grown in the laboratory and then given to the patient by infusion. The CAR T cells are able to bind to an antigen on the cancer cells and kill them.
See Drugs Approved for Multiple Myeloma and Other Plasma Cell Neoplasms.
Radiation therapy
Radiation therapy is a cancer treatment that uses high-energy x-rays or other types of radiation to kill cancer cells or keep them from growing. External radiation therapy uses a machine outside the body to send radiation toward the area of the body with cancer.
Surgery
Surgery to remove the tumor may be done. After the doctor removes all the cancer that can be seen at the time of the surgery, some patients may be given radiation therapy after surgery to kill any cancer cells that are left. Treatment given after the surgery, to lower the risk that the cancer will come back, is called adjuvant therapy.
Watchful waiting
Watchful waiting is closely monitoring a patient's condition without giving any treatment until signs or symptoms appear or change.
New types of treatment are being tested in clinical trials.
This summary section describes treatments that are being studied in clinical trials. It may not mention every new treatment being studied. Information about clinical trials is available from the NCI website.
New combinations of therapies
Clinical trials are studying different combinations of immunotherapy, chemotherapy, steroid therapy, and drugs. New treatment regimens using selinexor are also being studied.
Treatment for plasma cell neoplasms may cause side effects.
For information about side effects caused by treatment for cancer, visit our Side Effects page.
Supportive care is given to lessen the problems caused by the disease or its treatment.
This therapy controls problems or side effects caused by the disease or its treatment, and improves quality of life. Supportive care is given to treat problems caused by multiple myeloma and other plasma cell neoplasms.
Supportive care may include the following:
- Plasmapheresis: If the blood becomes thick with extra antibody proteins and interferes with circulation, plasmapheresis is done to remove extra plasma and antibody proteins from the blood. In this procedure blood is removed from the patient and sent through a machine that separates the plasma (the liquid part of the blood) from the blood cells. The patient's plasma contains the unneeded antibodies and is not returned to the patient. The normal blood cells are returned to the bloodstream along with donated plasma or a plasma replacement. Plasmapheresis does not keep new antibodies from forming.
- Induction therapy with stem cell transplant: If amyloidosis occurs, treatment may include induction therapy followed by stem cell transplant using the patient's own stem cells.
- Immunotherapy: Immunotherapy with thalidomide, lenalidomide, or pomalidomide is given to treat amyloidosis.
- Targeted therapy: Targeted therapy with proteasome inhibitors is given to decrease how much immunoglobulin M is in the blood and treat amyloidosis. Targeted therapy with daratumumab is given with or without other drugs to treat amyloidosis. Targeted therapy with a monoclonal antibody is given to slow bone loss and reduce bone pain.
- Radiation therapy: Radiation therapy is given for bone lesions of the spine.
- Chemotherapy: Chemotherapy is given to reduce back pain from osteoporosis or compression fractures of the spine.
- Bisphosphonate therapy: Bisphosphonate therapy is given to slow bone loss and reduce bone pain. For more information on bisphosphonates and problems related to their use, see Oral Complications of Cancer Therapies.
Patients may want to think about taking part in a clinical trial.
For some patients, taking part in a clinical trial may be the best treatment choice. Clinical trials are part of the cancer research process. Clinical trials are done to find out if new cancer treatments are safe and effective or better than the standard treatment.
Many of today's standard treatments for cancer are based on earlier clinical trials. Patients who take part in a clinical trial may receive the standard treatment or be among the first to receive a new treatment.
Patients who take part in clinical trials also help improve the way cancer will be treated in the future. Even when clinical trials do not lead to effective new treatments, they often answer important questions and help move research forward.
Patients can enter clinical trials before, during, or after starting their cancer treatment.
Some clinical trials only include patients who have not yet received treatment. Other trials test treatments for patients whose cancer has not gotten better. There are also clinical trials that test new ways to stop cancer from recurring (coming back) or reduce the side effects of cancer treatment.
Clinical trials are taking place in many parts of the country. Information about clinical trials supported by NCI can be found on NCI's clinical trials search webpage. Clinical trials supported by other organizations can be found on the ClinicalTrials.gov website.
Follow-up tests may be needed.
As you go through treatment, you will have follow-up tests or check-ups. Some tests that were done to diagnose or stage the cancer may be repeated to see how well the treatment is working. Decisions about whether to continue, change, or stop treatment may be based on the results of these tests.
Some of the tests will continue to be done from time to time after treatment has ended. The results of these tests can show if your condition has changed or if the cancer has recurred (come back).
Treatment of Monoclonal Gammopathy of Undetermined Significance
For information about the treatments listed below, see the Treatment Option Overview section.
Treatment of monoclonal gammopathy of undetermined significance (MGUS) is usually watchful waiting. Regular blood tests to check the level of M protein in the blood and physical exams to check for signs or symptoms of cancer will be done.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of Isolated Plasmacytoma of Bone
For information about the treatments listed below, see the Treatment Option Overview section.
Treatment of isolated plasmacytoma of bone is usually radiation therapy to the bone lesion.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of Extramedullary Plasmacytoma
For information about the treatments listed below, see the Treatment Option Overview section.
Treatment of extramedullary plasmacytoma may include the following:
- Radiation therapy to the tumor and nearby lymph nodes.
- Surgery, usually followed by radiation therapy.
- Watchful waiting after initial treatment, followed by radiation therapy, surgery, or chemotherapy if the tumor grows or causes signs or symptoms.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of Multiple Myeloma
For information about the treatments listed below, see the Treatment Option Overview section.
Patients without signs or symptoms may not need treatment. These patients can have watchful waiting until signs or symptoms appear.
When signs or symptoms appear, there are two categories for patients receiving treatment:
- Younger, fit patients who are eligible for a stem cell transplant.
- Older, unfit patients who are not eligible for a stem cell transplant.
Patients younger than 65 years are usually considered younger and fit. Patients older than 75 years are usually not eligible for a stem cell transplant. For patients between the ages of 65 and 75 years, fitness is determined by their overall health and other factors.
The treatment of multiple myeloma is usually done in phases:
Induction therapy: This is the first phase of treatment. Its goal is to reduce the amount of disease, and may include one or more of the following:- For younger, fit patients (eligible for a transplant):
- Chemotherapy.
- Targeted therapy with a proteasome inhibitor (bortezomib) and a monoclonal antibody (daratumumab).
- Immunotherapy (lenalidomide).
- Corticosteroid therapy (dexamethasone).
- For older, unfit patients (not eligible for a transplant):
- Chemotherapy.
- Targeted therapy with a proteasome inhibitor (bortezomib or carfilzomib) or a monoclonal antibody (daratumumab).
- Immunotherapy (lenalidomide).
- Corticosteroid therapy (dexamethasone).
|
Consolidation therapy: This is the second phase of treatment. Treatment in the consolidation phase is to kill any remaining cancer cells. High-dose chemotherapy is followed by either:- one autologous stem cell transplant, in which the patient's stem cells from the blood or bone marrow are used; or
- two autologous stem cell transplants followed by an autologous or allogeneic stem cell transplant, in which the patient receives stem cells from the blood or bone marrow of a donor; or
- one allogeneic stem cell transplant.
|
Maintenance therapy: After the initial treatment, maintenance therapy is often given to help keep the disease in remission for a longer time. Several types of treatment are being studied for this use, including the following:- Chemotherapy.
- Immunotherapy (lenalidomide).
- Corticosteroid therapy (prednisone or dexamethasone).
- Targeted therapy with a proteasome inhibitor (bortezomib or ixazomib) or a monoclonal antibody (daratumumab).
|
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Treatment of Relapsed or Refractory Multiple Myeloma
For information about the treatments listed below, see the Treatment Option Overview section.
Treatment of relapsed or refractory multiple myeloma may include the following:
- Watchful waiting for patients whose disease is stable.
- A different treatment than treatment already given, for patients whose tumor kept growing during treatment. See Multiple Myeloma treatment options.
- The same drugs used before the relapse may be used if the relapse occurs one or more years after initial treatment. See Multiple Myeloma treatment options.
Drugs used may include the following:
- Targeted therapy with monoclonal antibodies (daratumumab, elotuzumab, or isatuximab).
- Targeted therapy with proteasome inhibitors (bortezomib, carfilzomib, or ixazomib).
- Immunotherapy (pomalidomide, lenalidomide, or thalidomide).
- Chemotherapy.
- Corticosteroid therapy.
- A clinical trial of CAR T-cell therapy.
- A clinical trial of targeted therapy with a small molecule inhibitor (selinexor) and corticosteroid therapy.
- A clinical trial of targeted therapy with a BCL2 inhibitor (venetoclax).
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
To Learn More About Plasma Cell Neoplasms
For more information from the National Cancer Institute about multiple myeloma and other plasma cell neoplasms, see the following:
For general cancer information and other resources from the National Cancer Institute, visit:
About This PDQ Summary
About PDQ
Physician Data Query (PDQ) is the National Cancer Institute's (NCI's) comprehensive cancer information database. The PDQ database contains summaries of the latest published information on cancer prevention, detection, genetics, treatment, supportive care, and complementary and alternative medicine. Most summaries come in two versions. The health professional versions have detailed information written in technical language. The patient versions are written in easy-to-understand, nontechnical language. Both versions have cancer information that is accurate and up to date and most versions are also available in Spanish.
PDQ is a service of the NCI. The NCI is part of the National Institutes of Health (NIH). NIH is the federal government's center of biomedical research. The PDQ summaries are based on an independent review of the medical literature. They are not policy statements of the NCI or the NIH.
Purpose of This Summary
This PDQ cancer information summary has current information about treatment of plasma cell neoplasms (including multiple myeloma). It is meant to inform and help patients, families, and caregivers. It does not give formal guidelines or recommendations for making decisions about health care.
Reviewers and Updates
Editorial Boards write the PDQ cancer information summaries and keep them up to date. These Boards are made up of experts in cancer treatment and other specialties related to cancer. The summaries are reviewed regularly and changes are made when there is new information. The date on each summary ("Updated") is the date of the most recent change.
The information in this patient summary was taken from the health professional version, which is reviewed regularly and updated as needed, by the PDQ Adult Treatment Editorial Board.
Clinical Trial Information
A clinical trial is a study to answer a scientific question, such as whether one treatment is better than another. Trials are based on past studies and what has been learned in the laboratory. Each trial answers certain scientific questions in order to find new and better ways to help cancer patients. During treatment clinical trials, information is collected about the effects of a new treatment and how well it works. If a clinical trial shows that a new treatment is better than one currently being used, the new treatment may become "standard." Patients may want to think about taking part in a clinical trial. Some clinical trials are open only to patients who have not started treatment.
Clinical trials can be found online at NCI's website. For more information, call the Cancer Information Service (CIS), NCI's contact center, at 1-800-4-CANCER (1-800-422-6237).
Permission to Use This Summary
PDQ is a registered trademark. The content of PDQ documents can be used freely as text. It cannot be identified as an NCI PDQ cancer information summary unless the whole summary is shown and it is updated regularly. However, a user would be allowed to write a sentence such as "NCI's PDQ cancer information summary about breast cancer prevention states the risks in the following way: [include excerpt from the summary]."
The best way to cite this PDQ summary is:
PDQ® Adult Treatment Editorial Board. PDQ Plasma Cell Neoplasms (Including Multiple Myeloma) Treatment. Bethesda, MD: National Cancer Institute. Updated <MM/DD/YYYY>. Available at: https://www.cancer.gov/types/myeloma/patient/myeloma-treatment-pdq. Accessed <MM/DD/YYYY>. [PMID: 26389437]
Images in this summary are used with permission of the author(s), artist, and/or publisher for use in the PDQ summaries only. If you want to use an image from a PDQ summary and you are not using the whole summary, you must get permission from the owner. It cannot be given by the National Cancer Institute. Information about using the images in this summary, along with many other images related to cancer can be found in Visuals Online. Visuals Online is a collection of more than 3,000 scientific images.
Disclaimer
The information in these summaries should not be used to make decisions about insurance reimbursement. More information on insurance coverage is available on Cancer.gov on the Managing Cancer Care page.
Contact Us
More information about contacting us or receiving help with the Cancer.gov website can be found on our Contact Us for Help page. Questions can also be submitted to Cancer.gov through the website's E-mail Us.
Last Revised: 2023-11-17
If you want to know more about cancer and how it is treated, or if you wish to know about clinical trials for your type of cancer, you can call the NCI's Cancer Information Service at 1-800-422-6237, toll free. A trained information specialist can talk with you and answer your questions.